The following is an article written for the online, video-based physical therapy continuing education company MedBridge…
Stress fractures are a common occurrence amongst the military, cross country, and endurance athlete population patient populations. With the prospective studies indicating an incidence of 31% in military personnel and 21% in track and field athletes, this is an area that needs to be thoroughly understood by clinicians working in a direct access environment. While femoral stress fractures only account for 5-7% of all stress fractures, there is currently no validated clinical decision rule in identifying those at risk and therefore other factors need to be considered by the clinician. (Weishaar et al., 2005; Bennell et al., 1996; Milgrom et al., 1985; Matheson et al., 1987; Monteleone et al., 1995; Changstrom et al., 2014)
What causes a femoral stress fractures?
Stress-related bone and soft-tissue injuries occur in response to an excessive progression of repetitive loading activities. These injuries develop when the extent of the micro-damage exceeds the ability of the remodeling process to keep up with the demands placed upon it. With regards to femoral stress fractures, during running, the largest bending moments about the anterior to posterior axes of the proximal femur occurs during the impact phase of loading response. As this occurs, the largest stress is then placed on the medial aspect of the femur (Edwards et al., 2008)
Who is at risk? (Wright et al., 2015; Bennell et al., 1999)
- Stress fracture injury rates are highest in girls cross country (10.6), girls gymnastics (7.4), and boys cross country (5.4)
- In endurance athletes, female sex (odds ratio = 2.31) and previous history of stress fracture (OR = 4.99) were found to be significant risk factors
- The presence of concomitant ipsilateral Femoroacetabular impingement demonstrates a higher incidence in both the general and military population (Goldin et al., 2015; Carey et al., 2013)
- Recent, sudden increase in training volume, especially in relatively inactive individuals
What is the clinical presentation? (Clement et al., 1993; Weishaar et al., 2005; Wright et al., 2015)
- Vague pain in the thigh that radiates into the hip and/or groin region
- Anterior thigh (45.9%), hip (27.0%), and/or groin (8.1%) pain
- In femoral shaft stress fractures, hip A/PROM not typically limited, but can be painful, however in femoral neck stress fractures, a gross limitation in A/PROM can be present
- Groin pain with single leg hop (70%)
Special Testing? (Reiman et al., 2012; Reiman et al., 2015)
1. Patellar-pubic Percussion Test
| Reliability | Sensitivity | Specificity | +LR | -LR |
| 0.89 | 0.89 – 0.96 | 0.82 – 0.95 | 5.1 – 20.4 | 0.06 – 0.75 |
2. Fulcrum Test
| Reliability | Sensitivity | Specificity | +LR | -LR |
| N/A | 1.00 | 1.00 | ∞ | 0.00 |
Is conservative management effective?
There have been several case reports and case series detailing successful diagnosis, treatment, and return to sport following conservative management. Unfortunately, at this time, there have been no high-level studies supporting the physical therapy intervention in this population. In those case studies detailing successful management, programs included progressive posterolateral hip strengthening, neuromuscular re-education, and a graded return to running/physical activity (Weishaar et al., 2005; Ivkovic et al., 2006; Kang et al., 2005).
Without the clinical decision rules for identification of fracture that are available for the foot/ankle (Ottawa Ankle Rules), knee (Ottawa Knee Rules, Pittsburgh Knee Rules), and cervical spine (Canadian Cervical Spine Rules), evaluation of potential hip fracture needs to be managed with the best available evidence. By taking into consideration patient demographics, subjective report of training volume/progression, and utilizing tests/measures supported in the literature, the treating clinician can more accurately identify those athletes in need of further radiological evaluation.
Continued Reading…

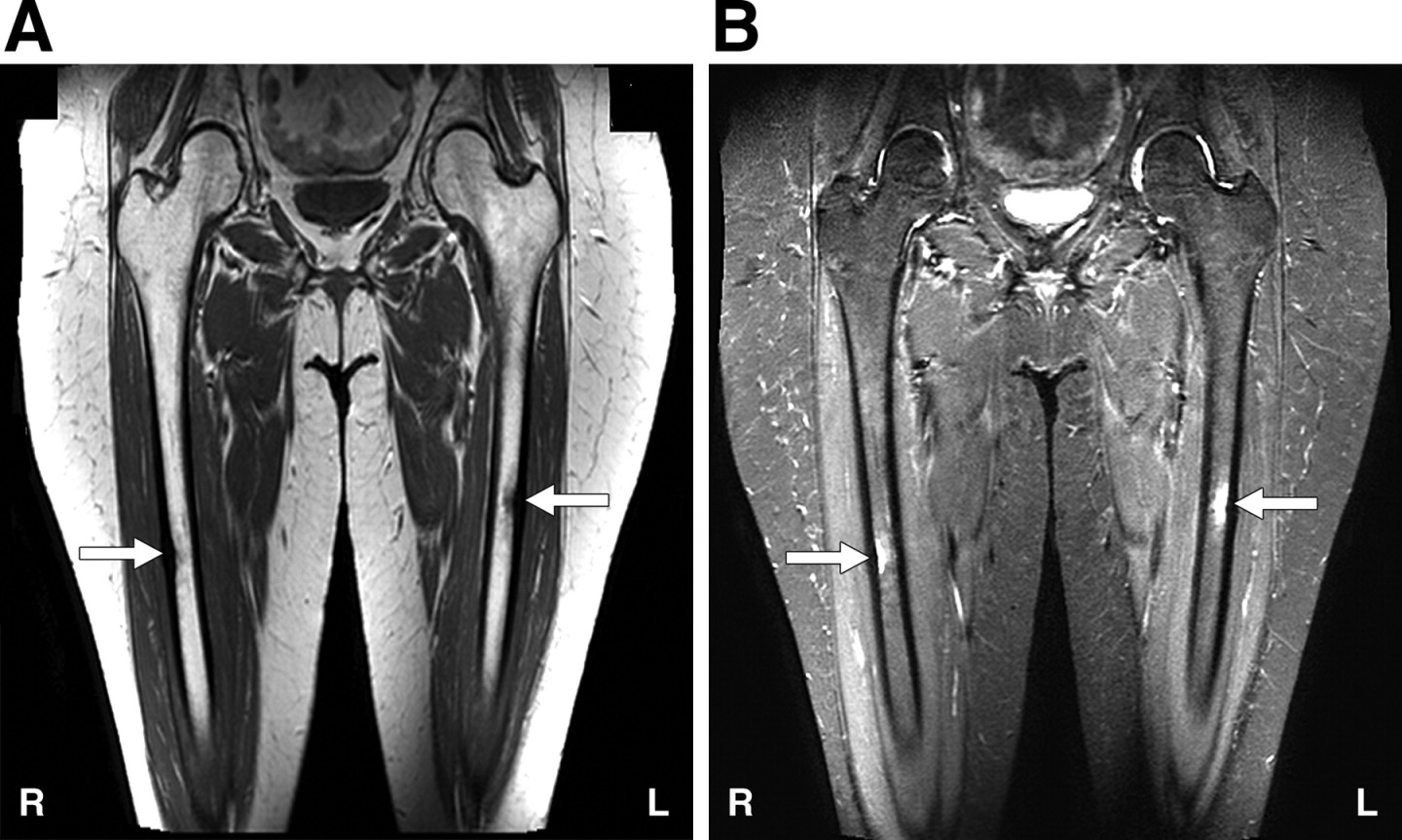




Any vague pain after strenuous activity at hip joint & thigh should be taken as stress fracture till proved otherwise. And immediate rest is mandatory.
LikeLike